Being 42 and pregnant is not necessarily a combination I would recommend. Two years ago I ran a marathon in Athens, Greece; two hours ago I managed to walk 4 blocks from my chiropractor's office back to our house...and felt proud to accomplish that much after this week of woe.
Usually my pregnancies are pretty "easy." Oh, sure, I've dealt with some small issues here and there (early pregnancy nausea, some heartburn, swelling) and of course the inevitable feeling-like-a-whale, grunting-when-rising, awkwardly-flopping-about phase that means Baby's due date is approaching (although not soon enough for my liking).
But this...? My 11th pregnancy, the 9th one to make it past the first trimester...this pregnancy takes the cake for physical difficulties. Let's be real: it was a number of pregnancies ago when I realized that being pregnant in my 30s was much harder than in my 20s! And in my 40s?! Good heavens! I thought the varicose veins and swelling I dealt with during Rhema's (Baby #8) pregnancy were pretty awful! Not surprisingly, the veins began bothering me again early on with Verity, and this time I took the time to get fitted for some quality compression stockings that have helped tremendously. In fact, one improvement is that I hardly ever have any swelling. Yahoo for that!
Unfortunately, the combination of my age plus the T18 diagnosis has me a bit on edge, so when I experience what is for me a new and unusual form of pain or discomfort, I'm never quite sure whether it's something I just have to endure or whether it warrants further examination. Christmas Eve had me questioning some more experienced folks when the stabbing pains in my right leg (the one with the lovely varicose veins) were sharp enough to reduce me to tears. Based on input from some nurse friends, we decided I should head to the emergency room (because of course these things happen on the weekends when the military clinic is closed) to get checked out, just in case deep vein thrombosis was the cause.
Knowing I was likely to be "occupied" for a number of hours, I chose to drive myself and have Ted stay home with the kids. I left the house around 11am, all my hopes and plans for a lovely, family-centered Christmas Eve crashing down as I took a small packed lunch, water bottles, and some reading material...Rick and Karen Santorum's account of having a little girl, Bella, with trisomy 18. Bella's Gift is a beautifully written and brutally honest love story.
I was glad for the book...I waited in the waiting room nearly an hour and a half, and then I was in the ER exam room for about 4 hours. I quickly learned that I needed to MOVE every 10 minutes or so; I couldn't stay sitting or lying very long without the stabbing pains bothering me. So I rotated between the bed (leg elevated) to pacing my room a bit to sitting awhile to pacing the room...and so on.
In between all of this I saw actual people from time to time, lol! Eventually I got blood drawn to determine whether it was "thicker" than normal to see if there was a concern for clotting. Apparently that was the case, because then the next step was meeting the Venous Doppler machine and the friendly tech who accompanied it. She did her job well, but I nearly passed out when she had to scan the painful parts on my lower leg! My blood pressure dropped and there was a bit of a stir, but before too long I was back to normal and hearing from the doctor that, PRAISE GOD, I did NOT have DVT but only superficial clotting (sometimes called phlebitis). I was released soon after that with instructions for home care plus a prescription for some pain killers...which was all but useless since it was Christmas Eve night by this point and nothing was open!
I made the drive back to our little town in time to join the family for the Christmas Eve sermon delivered by our pastor, having just missed the music portion during which our oldest daughter played the violin for the first time in a non-recital setting. Sigh. Thankfully her dad captured the songs on video, and she did fantastic!! So proud of my beautiful girl!
My leg pain forced a much simpler Christmas than I may have desired...even though we had already been planning for a simpler family celebration. My wonderful family pitched in to prepare various parts of the meal, and it was a memorable day even though (for me) a good portion was spent trying to prop my leg and keep moist heat on it.
After a few days, the pain from the clotting was greatly subsiding...but yesterday morning I awoke with a severe Charlie-horse spasm in my hamstring of all places. (Same leg as the varicose veins and clots--oh, joy!) The spasms were nearly non-stop allllllll day. The only relief I experienced happened during my two Epsom salt baths, one after lunch and one before bedtime. Today the spasms seem to have stopped--mostly--occurring only when I transition from sitting to standing or vice versa instead of continuously. The muscles all up the back of my right leg are extremely tender. My husband and I went to the chiropractor this morning, and I decided to try walking home slowly. I would not have been able to do that yesterday, so there is definitely improvement...but I feel like an old woman! Between the rotating use of heat packs and essential oils and pain relief cream, I am feeling far beyond these 42 years.
This pregnancy has been so hard on my body.
But it has also been extremely hard on my heart.
Some days it is difficult to say which is the worse for the wear...
My soul melts away for sorrow; strengthen me according to your word!
This is my comfort in my affliction, that your promise gives me life. (Psalm 119:28, 50 ESV)
Thursday, December 29, 2016
Tuesday, December 27, 2016
December Check-up and Ultrasound
I'm a bit behind in posting--not surprising, given the time of year!
On December 9 I had my monthly OB check with yet another pregnant military doctor, lol. She was due within 3 weeks, so I'm assuming I won't see her again! I took along a little heart-shaped recorder to capture Verity's heartbeat in recorded form. The kids were delighted with this little treasure (part of a keepsake box so thoughtfully sent to us by a beautiful organization, String of Pearls)...a bit too much so! I had to put it away before Rhema or Seanin made off with it! There was not a lot of information to be gained from this appointment, though one of my questions about the previous ultrasound was answered: I had been wondering about the level of amniotic fluid (it can often be high with T18 babies) and learned that it was high but not out of the "normal" range. We decided to go ahead and schedule one more appointment for me at the military base (set for January 9), after which point I will start having my check-ups every two weeks at the university medical center where we get our ultrasounds done.
Our last peek at Verity was December 20. Ted was able to leave work early enough to meet me at the center; he had missed the November ultrasound, but my mom and Charis were there with me that time.
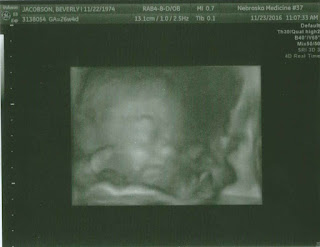
Our tech was extremely bubbly and so sweet! She printed out tons of pictures for us, gave us multiple looks at Verity in 3D, and exclaimed over every little positive thing. She was exemplary in her treatment of us and our little girl! Here are some views of Verity at 30 weeks, 3 days:
In November Verity was measuring in the 7th percentile; this month she was down to the 4th. Obviously this is compared to all other babies, most of whom are "normal." So I was excited that this time, we had some extra information on hand: a "growth chart" of sorts for trisomy 18 babies. It shows birth weights at different gestational weeks, dividing the girls from the boys and showing a ranking within T18 babies. Based on THIS information, Verity's 2 pounds, 13 ounces (or 1264 grams, if I remember correctly) has her weighing in at the 50th-70th percentile when compared to other trisomy 18 baby girls. Granted, the numbers from this pool are pretty small, maybe 25+ babies at the 30-week mark and about 15 at 31 weeks. (We were kind of in the middle so looked at both sets of numbers, but either way Verity ranked in the middle for size.)
The doctor who spoke with us this time was a new face, but he was kind enough...he didn't really give us any new information. I almost feel that we are at the point where WE may very well have more information than our medical caregivers, so I am going to be sure to carry copies of the research articles I've been reading (see previous two posts) to give out as needed. (Our genetic counselor was delighted to see us again and receive copies of them when she visited our exam room just before the ultrasound!)
Next ultrasound is January 13. I was pretty content to have scans done every 4 weeks or so, because I wasn't convinced there would be any benefit to doing them more often. (We aren't monitoring her heart, for example.) However...when I saw someone comment about the importance of weekly scans on the trisomy parent Facebook page I keep up with, I asked why. This is the response I received:
"If the baby has trisomy 18, that means the placenta also has the faulty chromosomal makeup, and often the placenta fails first and then the baby passes in the womb. They will Doppler the cord flow from placenta to baby to see if it's elevated at all or restricting oxygen. If the baby is going to pass in the womb or something go wrong, it can be caught first by watching the placenta to the baby!"
So this has given me something new to consider. So far, however, things have looked very good, and Verity is an incredibly active baby--possibly even more so than my others! Now I'm praying for wisdom to know if we should increase the monitoring in the future. The med center has offered to do more frequent scans, though the doctors have all indicated they don't think it's necessary. (Not that--we've learned--we want to rely on what the doctors think is or isn't necessary for a trisomy 18 baby!)
On December 9 I had my monthly OB check with yet another pregnant military doctor, lol. She was due within 3 weeks, so I'm assuming I won't see her again! I took along a little heart-shaped recorder to capture Verity's heartbeat in recorded form. The kids were delighted with this little treasure (part of a keepsake box so thoughtfully sent to us by a beautiful organization, String of Pearls)...a bit too much so! I had to put it away before Rhema or Seanin made off with it! There was not a lot of information to be gained from this appointment, though one of my questions about the previous ultrasound was answered: I had been wondering about the level of amniotic fluid (it can often be high with T18 babies) and learned that it was high but not out of the "normal" range. We decided to go ahead and schedule one more appointment for me at the military base (set for January 9), after which point I will start having my check-ups every two weeks at the university medical center where we get our ultrasounds done.
Our last peek at Verity was December 20. Ted was able to leave work early enough to meet me at the center; he had missed the November ultrasound, but my mom and Charis were there with me that time.
Our tech was extremely bubbly and so sweet! She printed out tons of pictures for us, gave us multiple looks at Verity in 3D, and exclaimed over every little positive thing. She was exemplary in her treatment of us and our little girl! Here are some views of Verity at 30 weeks, 3 days:
 |
| You can see the cord floating in front of her face, but I love her little nose! Also you can see a bit of fat on her cheeks and those adorable lips. |
 |
| She is showing us her bicep, lol! Precious little fist up by her forehead. The shadowy thing across her nose is the cord; the tech was able to "erase" part of it. |
 |
| Did you know you can see hair on an ultrasound?! I didn't! This is the top of Verity's head, easily seen by the outline. But at the back...little hairs! |
 |
| Verity's profile at 30 weeks, 3 days. The "bubble" over her nose is the umbilical cord. |
In November Verity was measuring in the 7th percentile; this month she was down to the 4th. Obviously this is compared to all other babies, most of whom are "normal." So I was excited that this time, we had some extra information on hand: a "growth chart" of sorts for trisomy 18 babies. It shows birth weights at different gestational weeks, dividing the girls from the boys and showing a ranking within T18 babies. Based on THIS information, Verity's 2 pounds, 13 ounces (or 1264 grams, if I remember correctly) has her weighing in at the 50th-70th percentile when compared to other trisomy 18 baby girls. Granted, the numbers from this pool are pretty small, maybe 25+ babies at the 30-week mark and about 15 at 31 weeks. (We were kind of in the middle so looked at both sets of numbers, but either way Verity ranked in the middle for size.)
The doctor who spoke with us this time was a new face, but he was kind enough...he didn't really give us any new information. I almost feel that we are at the point where WE may very well have more information than our medical caregivers, so I am going to be sure to carry copies of the research articles I've been reading (see previous two posts) to give out as needed. (Our genetic counselor was delighted to see us again and receive copies of them when she visited our exam room just before the ultrasound!)
Next ultrasound is January 13. I was pretty content to have scans done every 4 weeks or so, because I wasn't convinced there would be any benefit to doing them more often. (We aren't monitoring her heart, for example.) However...when I saw someone comment about the importance of weekly scans on the trisomy parent Facebook page I keep up with, I asked why. This is the response I received:
"If the baby has trisomy 18, that means the placenta also has the faulty chromosomal makeup, and often the placenta fails first and then the baby passes in the womb. They will Doppler the cord flow from placenta to baby to see if it's elevated at all or restricting oxygen. If the baby is going to pass in the womb or something go wrong, it can be caught first by watching the placenta to the baby!"
So this has given me something new to consider. So far, however, things have looked very good, and Verity is an incredibly active baby--possibly even more so than my others! Now I'm praying for wisdom to know if we should increase the monitoring in the future. The med center has offered to do more frequent scans, though the doctors have all indicated they don't think it's necessary. (Not that--we've learned--we want to rely on what the doctors think is or isn't necessary for a trisomy 18 baby!)
Saturday, December 17, 2016
Verity Is Our Baby...Not a Diagnosis
Understatement: Continuing a pregnancy with a high risk of miscarriage or stillbirth is a difficult, emotional journey. It is even more complicated when considering that should the baby survive birth, he or she will have special needs and a shortened life span, even if "exceeding expectations."
As my husband and I have learned from personal experience, the input we receive from medical professionals along our journey contributes in a huge way to either lightening our burdens or adding to them. The research article I want to highlight today is titled "Our Children Are Not a Diagnosis" (full citation at the end of this post), and the pointers offered to health care providers (HCPs) rang so true when I read them that I felt the information was worth shouting to the world!
First, I want to share some feelings and experiences common to parents who choose to continue pregnancies despite diagnoses of fetal anomalies. Since the research represented input from parents of 107 children with full T13 or T18, I feel we are in good company, with many of the quotes and answers resonating with our personal feelings and experience. Quotes from the article are in italics; I will follow with commentary about our own experience.
Facts:
Guon J, Wilfond BS, Farlow B, Brazg T, Janvier A, 2013. Our children are not a diagnosis: The experience of parents who continue their pregnancy after a prenatal diagnosis of trisomy 13 or 18. Am J Med Genet Part A 9999:1-11.
As my husband and I have learned from personal experience, the input we receive from medical professionals along our journey contributes in a huge way to either lightening our burdens or adding to them. The research article I want to highlight today is titled "Our Children Are Not a Diagnosis" (full citation at the end of this post), and the pointers offered to health care providers (HCPs) rang so true when I read them that I felt the information was worth shouting to the world!
First, I want to share some feelings and experiences common to parents who choose to continue pregnancies despite diagnoses of fetal anomalies. Since the research represented input from parents of 107 children with full T13 or T18, I feel we are in good company, with many of the quotes and answers resonating with our personal feelings and experience. Quotes from the article are in italics; I will follow with commentary about our own experience.
Facts:
- "Parents experience intense grief reactions regardless of the choice they make. However, parents who were offered support and who chose to continue pregnancy described a positive experience in all explorative descriptive studies."
- "The majority of parents felt some HCPs did not view children with T13-18 as unique children and that they did not look beyond the grim statistics of these conditions." [This has been true of two of the doctors we have consulted with at various times--but not of the providers I have seen at the military treatment facility.] After diagnosis, parents report being told that:
- Their baby would likely die before or at the time of birth [Check]
- Their baby would not live more than a few months [Check]
- The condition of their baby was lethal or incompatible with life [Insinuated if not in these words]
- Their child would be a vegetable [The actual word spoken to me was "retarded."]
- Their baby would destroy their family or their marriage [Check]
- If their baby survived, he would live a meaningless life or a life of suffering [The word used here was "futile."]
- "The majority (61%) of parents reported feeling pressure to terminate their pregnancy." [I am pleased to say that none of the HCPs I have spoken with either in person or on the phone has even suggested this, but this perhaps may have been different if we had not begun EVERY meeting by firmly telling that particular HCP that abortion is NOT an option for us.]
- When first hearing about the diagnosis, "The most common hope was that the child would be born alive and that parents would have a modest amount of time to spend with their child.... Parents report understanding the implications of the diagnosis and only a few had hopes for a miracle or a cure. These modest hopes reflected acceptance of the serious condition." [This is certainly true for us. I don't want or need HCPs to paint a rosy picture for us. We are well aware of the facts. I DO want them to understand the not-so-negative facts, though.]
Ideally, parents who receive a prenatal diagnosis should also receive the full range of information, including new data about these conditions. The spectrum of outcomes for T13 and T18 babies is extremely wide. With a disproportionately high number of these babies being aborted, the statistics we do have are already skewed. But while the traditional view is to describe these conditions as "lethal" or "incompatible with life," the truth is that when interventions are provided, particularly for those who do not have severe anomalies, the one-year survival rates have been reported to be as high as 56% (in some Japanese studies). And as I learned from the article referenced in my last post, early interventions can make a huge difference in how long a T13 or T18 baby lives after birth. It is true that life spans are still significantly shorter, with a small percentage making it past one year. But why not allow parents the opportunity to make and cherish precious memories no matter how long their child lives?
The article featured in this post concludes with the paragraph below, followed by a list of suggestions to assist HCPs in providing optimal prenatal care. I encourage you to share this post or these suggestions with anyone you know in the medical field; it is obvious that some of the doctors I have seen have not encountered a trisomy 18 pregnancy, and they just aren't sure what to tell me other than parroting the statistics that indicate our daughter will likely die sooner rather than later. In general they are kind, compassionate, and non-judgmental; but neither do they understand that T18 isn't necessarily an IMMEDIATE death sentence. I hope to provide people like them with information that gives a fuller picture of the range of possibilities.
"HCPs need to understand parental perspectives and realize that while T13-18 cannot be 'cured,' the children have value and meaning to their parents regardless of life span and disability. HCPs can provide many positive actions to prepare parents for the life or death of their child. All these interventions result in a measure of 'healing' without cure. Pictures are worth a thousand words. The contrast between family pictures and the pictures of children with trisomy 13 and 18 found in medical texts is striking and demonstrates the contrasting representations of children with these conditions....
Based on the information obtained in this study from parents who continued their pregnancy after a diagnosis of T13-18, we offer suggestions to assist health care providers to provide optimal prenatal care:
- At the time of diagnosis, provide accurate survival figures. Avoid words like "lethal," "incompatible with life," and "vegetable." Avoid value-laden language related to disability.
- Parents should be informed that most parents who choose to continue pregnancy have reported a positive and enriching experience regardless of the lifespan of their child.
- Parents who decide to continue their pregnancy need support, not judgment or pressure to change their choice. Parents accept that early death is likely and they have chosen to value the time they have, both before and after birth.
- Remember that to these parents, their child is a person, not a diagnosis. Refer to the unborn child by name, if possible. Parents expect to receive medical information related to their child, not to the diagnosis. Informing parents of normal organs in addition to anomalies is greatly appreciated. Offer hope when it is reasonable: hope that baby will continue to grow in utero, hope that baby will be born alive and that parents will enjoy some time with the baby.
- Offer to continue prenatal and fetal care as for any pregnancy. Ultrasounds are very special, memorable events and given the high risk of miscarriage, might be the only time parents will see their living baby. Taking a few minutes during the ultrasound to point out normal or "cute" features of the baby can be a lifetime gift to parents.
- Guide parents to create a birth plan that is best for their child and family. Parents should understand that children with T13 or 18 are unique and some might benefit from life-sustaining interventions while some may be harmed by them. Ensure that the birth plan includes collectibles for memories such as footprints and photographs. In indicated, be transparent with parents about any hospital protocol or policy that restricts certain interventions to babies born with T13-18. Parental challenges to these restrictions should be discussed in a multi-disciplinary meeting or ethics consultation.
- Most parents who choose to continue pregnancy do so because it is the better path according to their personal beliefs. They appreciate empathy and kindness on their extraordinarily difficult journey, especially recognition of and respect for their love for their child."
*************
NOTE: This post refers to and quotes the following article, noted in italic text throughout the post:
Guon J, Wilfond BS, Farlow B, Brazg T, Janvier A, 2013. Our children are not a diagnosis: The experience of parents who continue their pregnancy after a prenatal diagnosis of trisomy 13 or 18. Am J Med Genet Part A 9999:1-11.
Friday, December 16, 2016
The Drawbacks of a Prenatal Diagnosis
Yesterday I read some articles published in the American Journal of Medical Genetics. These were sent to me by a lady on the Rare Trisomy Parents Facebook group in response to some questions I had posted. As one of the co-authors and collaborators of these and other studies (not to mention the mother of a trisomy 13 daughter), Barb is kind of a go-to person on the parent page. I so appreciated the information she sent me. The studies were quite thorough and well-presented, with findings related to concrete statistics as well as open-ended input regarding parents' experiences and emotions. In this blog post, I want to highlight some specific information from an article titled "Parental Hopes, Interventions, and Survival of Neonates with Trisomy 13 and Trisomy 18" (full citation follows at the end of the post).
I sat down with a hot drink and highlighter in hand to carefully read the pages I had printed. I confess I was not prepared for what I felt was the most stunning finding of all. See what you think after reading this paragraph:
"The single most important factor independently related to mortality before going home or before one year, even when correcting for all other factors (including congenital anomalies, interventions, and palliative care), was the presence of a prenatal diagnosis."
A prenatal diagnosis?! Something I have been thankful for, the one thing we DO know with certainty--the knowledge during pregnancy that our daughter has full trisomy 18--that knowledge actually could have a negative effect?!
Wow. And yet, when I consider the words of the NICU doctor with whom I had a consultation, it completely makes sense. Hang with me and follow this train of thought: Parents, trusting health care professionals, receive information that may or may not be current...filtered through lenses of personal beliefs...relying on grim statistics that ignore (or are ignorant of) any positive outcomes...and under the influence of a variety within the health care field, accept sentiments that become a self-fulfilling prophecy and act accordingly.
The vast differences in outcomes and care plans for children with a prenatal vs. a postnatal diagnosis showed up in several ways. For those who had a prenatal diagnosis, the study found that parents have similar hopes; in fact, our personal answers fit right in with the general consensus of those who chose to carry their babies to term: "They hope to meet their child alive, take their child home, be a family and give their child a good life."
So what did medical providers recommend to these parents whose hopes are outlined thus?
"...the recommendations parents had from medical providers were homogeneous: comfort care at birth with the plan of not prolonging life was recommended to all parents."
Referring to other medical articles/resources, the authors of this study noted that these recommendations were probably based solely on the chromosomal diagnosis, as evidenced by many position statements, hospital policies and authors who consider that interventions for these conditions are futile. (There's that word again! "Futile." Used multiple times by the NICU doctor with whom I spoke.)
Postnatal diagnoses for the respondents in the study came an average of 6 days after birth. So any interventions came as a result of medical personnel doing their jobs:
"Children with a postnatal diagnosis received ventilator support according to their respiratory status only (and not related to decision-making or genetic label)."
Next, there was a clear difference even in what constituted "palliative care" for babies with a prenatal vs. postnatal diagnosis.
"It seems that palliative care, for children with prenatal diagnosis, is directed to a goal of having as short a survival as possible, with medications being prepared even before delivery. Giving the child an optimal death seemed to be the goal of palliative care after a prenatal diagnosis of trisomy 13 or 18."
On the other hand:
"For children with postnatal diagnosis, palliative care may involve numerous different neonatal interventions...[to include] transfusion for weakness and inability to feed, tube feeds for comfort, CPAP for dyspnea, surgical closure of meningomyelocele, surgery for omphalocele, ventriculo-peritoneal shunt, and even 'cardiac surgery for comfort' (symptomatic child with a VSD). It is likely that many pediatricians would not describe such interventions as palliative."
There is certainly a lot more I could write or quote, but I think you get the general idea. Having a prenatal diagnosis can actually be a lot more harmful than being blissfully unaware of a chromosomal issue until after the baby arrives and makes his or her needs known.
So...what does this mean for us as a family? Further, what does it mean for YOU, perhaps a friend of our family, or even a random stranger who stumbled upon this humble blog entry? Here are some things I've been pondering...
First, as a parent of a baby girl with a prenatal diagnosis of full trisomy 18, I feel extremely grateful to be acting on the offensive instead of the defensive. While so much is out of our control, and though many things are uncertain about Verity's physical and mental status, simply KNOWING that any medical providers we encounter at delivery are likely going to have similar biases going into L&D with us helps us prepare to communicate firmly and effectively.
Second, as I read more of how other parents dealt with decision-making and care plans for their children, I feel much comfort in the fact that Ted and I are in agreement with each other, and also the fact that our "game plan" looks pretty much like what I see outlined in the report:
"Decisions were influenced by the state of the child and whether he was vigorous or weak with parents in general not wanting to impose undue suffering. Parents of almost half the children discharged on comfort care later decided to consider surgical interventions, because their child exceeded expectations."
In the absence of any concrete information at this time, we have simply said that we will wait and see what Verity needs when she needs it. As our genetic counselor told us, "Verity herself will let us know what she needs when she's born!" We plan to give her whatever support she needs, particularly help with respiration and feeding, as those are common issues. Anything that will not cause her undue discomfort but enhance her ability to breathe and receive nourishment--that's a given. That's our first plan of action. And then we take one day at a time and see how she's doing.
Now...what can all of this mean for YOU--and bless you, if you are still reading! Well, I can only encourage you to be willing to share information as you have the opportunity. Many health care providers are stuck in the "dark ages" when it comes to a diagnosis such as trisomy 13 or 18. And since these are fairly rare issues, it stands to reason that the average parent will know very little as well. Maybe someday you will be in the position of sharing information with a distraught couple who needs to know truth?
"Based on our findings and the current literature, if a baby is born near term, with a weight above 2.5kg, without a complex congenital anomaly, the chances of survival to discharge and to one year of age are significant. Our data about ventilator support and early survival are important. Poor respiratory drive immediately after birth is common. This support can often be removed after a short time and allow survival to go home. Sometimes, prolonged survival occurs, especially in neonates without complex cardiac anomalies or other significant adverse associated diagnoses. Infants with a prenatal diagnosis generally do not receive ventilator support, unless parents decide for interventions before birth."
Verity seems to fit the description of a trisomy 18 baby who may very well "exceed expectations." She does not have any complex cardiac anomalies or other "significant adverse associated diagnoses." It makes me wonder how many other trisomy 18 babies might have stood a chance at beating the odds and allowing their parents more time to spend with them on earth...if only they had had the opportunity for care before receiving a diagnosis. As the article queried, "It is important to examine decisions to withhold/withdraw interventions and whether they are in the best interest of neonates and whether our goal for these children is a good death, or is it a good life?"
Janvier A, Farlow B, Barrington KJ. 2016. Parental hopes, interventions, and survival of neonates with trisomy 13 and trisomy 18. Am J Med Genet Part C Semin Med Genet 999C:1-9.
I sat down with a hot drink and highlighter in hand to carefully read the pages I had printed. I confess I was not prepared for what I felt was the most stunning finding of all. See what you think after reading this paragraph:
"The single most important factor independently related to mortality before going home or before one year, even when correcting for all other factors (including congenital anomalies, interventions, and palliative care), was the presence of a prenatal diagnosis."
A prenatal diagnosis?! Something I have been thankful for, the one thing we DO know with certainty--the knowledge during pregnancy that our daughter has full trisomy 18--that knowledge actually could have a negative effect?!
Wow. And yet, when I consider the words of the NICU doctor with whom I had a consultation, it completely makes sense. Hang with me and follow this train of thought: Parents, trusting health care professionals, receive information that may or may not be current...filtered through lenses of personal beliefs...relying on grim statistics that ignore (or are ignorant of) any positive outcomes...and under the influence of a variety within the health care field, accept sentiments that become a self-fulfilling prophecy and act accordingly.
The vast differences in outcomes and care plans for children with a prenatal vs. a postnatal diagnosis showed up in several ways. For those who had a prenatal diagnosis, the study found that parents have similar hopes; in fact, our personal answers fit right in with the general consensus of those who chose to carry their babies to term: "They hope to meet their child alive, take their child home, be a family and give their child a good life."
So what did medical providers recommend to these parents whose hopes are outlined thus?
"...the recommendations parents had from medical providers were homogeneous: comfort care at birth with the plan of not prolonging life was recommended to all parents."
Referring to other medical articles/resources, the authors of this study noted that these recommendations were probably based solely on the chromosomal diagnosis, as evidenced by many position statements, hospital policies and authors who consider that interventions for these conditions are futile. (There's that word again! "Futile." Used multiple times by the NICU doctor with whom I spoke.)
Postnatal diagnoses for the respondents in the study came an average of 6 days after birth. So any interventions came as a result of medical personnel doing their jobs:
"Children with a postnatal diagnosis received ventilator support according to their respiratory status only (and not related to decision-making or genetic label)."
Next, there was a clear difference even in what constituted "palliative care" for babies with a prenatal vs. postnatal diagnosis.
"It seems that palliative care, for children with prenatal diagnosis, is directed to a goal of having as short a survival as possible, with medications being prepared even before delivery. Giving the child an optimal death seemed to be the goal of palliative care after a prenatal diagnosis of trisomy 13 or 18."
On the other hand:
"For children with postnatal diagnosis, palliative care may involve numerous different neonatal interventions...[to include] transfusion for weakness and inability to feed, tube feeds for comfort, CPAP for dyspnea, surgical closure of meningomyelocele, surgery for omphalocele, ventriculo-peritoneal shunt, and even 'cardiac surgery for comfort' (symptomatic child with a VSD). It is likely that many pediatricians would not describe such interventions as palliative."
There is certainly a lot more I could write or quote, but I think you get the general idea. Having a prenatal diagnosis can actually be a lot more harmful than being blissfully unaware of a chromosomal issue until after the baby arrives and makes his or her needs known.
So...what does this mean for us as a family? Further, what does it mean for YOU, perhaps a friend of our family, or even a random stranger who stumbled upon this humble blog entry? Here are some things I've been pondering...
First, as a parent of a baby girl with a prenatal diagnosis of full trisomy 18, I feel extremely grateful to be acting on the offensive instead of the defensive. While so much is out of our control, and though many things are uncertain about Verity's physical and mental status, simply KNOWING that any medical providers we encounter at delivery are likely going to have similar biases going into L&D with us helps us prepare to communicate firmly and effectively.
Second, as I read more of how other parents dealt with decision-making and care plans for their children, I feel much comfort in the fact that Ted and I are in agreement with each other, and also the fact that our "game plan" looks pretty much like what I see outlined in the report:
"Decisions were influenced by the state of the child and whether he was vigorous or weak with parents in general not wanting to impose undue suffering. Parents of almost half the children discharged on comfort care later decided to consider surgical interventions, because their child exceeded expectations."
In the absence of any concrete information at this time, we have simply said that we will wait and see what Verity needs when she needs it. As our genetic counselor told us, "Verity herself will let us know what she needs when she's born!" We plan to give her whatever support she needs, particularly help with respiration and feeding, as those are common issues. Anything that will not cause her undue discomfort but enhance her ability to breathe and receive nourishment--that's a given. That's our first plan of action. And then we take one day at a time and see how she's doing.
Now...what can all of this mean for YOU--and bless you, if you are still reading! Well, I can only encourage you to be willing to share information as you have the opportunity. Many health care providers are stuck in the "dark ages" when it comes to a diagnosis such as trisomy 13 or 18. And since these are fairly rare issues, it stands to reason that the average parent will know very little as well. Maybe someday you will be in the position of sharing information with a distraught couple who needs to know truth?
"Based on our findings and the current literature, if a baby is born near term, with a weight above 2.5kg, without a complex congenital anomaly, the chances of survival to discharge and to one year of age are significant. Our data about ventilator support and early survival are important. Poor respiratory drive immediately after birth is common. This support can often be removed after a short time and allow survival to go home. Sometimes, prolonged survival occurs, especially in neonates without complex cardiac anomalies or other significant adverse associated diagnoses. Infants with a prenatal diagnosis generally do not receive ventilator support, unless parents decide for interventions before birth."
Verity seems to fit the description of a trisomy 18 baby who may very well "exceed expectations." She does not have any complex cardiac anomalies or other "significant adverse associated diagnoses." It makes me wonder how many other trisomy 18 babies might have stood a chance at beating the odds and allowing their parents more time to spend with them on earth...if only they had had the opportunity for care before receiving a diagnosis. As the article queried, "It is important to examine decisions to withhold/withdraw interventions and whether they are in the best interest of neonates and whether our goal for these children is a good death, or is it a good life?"
******************
NOTE: This post refers to and quotes the following article, noted in italic text throughout the post:Janvier A, Farlow B, Barrington KJ. 2016. Parental hopes, interventions, and survival of neonates with trisomy 13 and trisomy 18. Am J Med Genet Part C Semin Med Genet 999C:1-9.
Labels:
Diagnosis,
Hope,
Medical Input,
Research,
Trisomy 13,
Trisomy 18,
Truth
Sunday, December 11, 2016
Holding Pattern
I've had some close friends ask lately how I'm doing. Most days the answer is, "Pretty well, actually." It's rather startling to realize how ordinary life seems after the tumultuous roller coaster of October and November.
I have somewhat arrogantly assumed that our holiday season will be "normal," untouched by drama or trauma. Maybe it's wishful thinking; maybe it's an unspoken prayer that God will give us some sweet, precious memories together before Whatever Happens Next swoops in and takes over our lives. I desperately want to foster a festive and generous holiday spirit in our hearts and in our home, particularly for our younger children who don't have as many Christmas memories racked up as their older siblings. (I recently overheard my three-year-old son listing objects on our Advent calendar, having learned at least a few things even though we haven't actually STARTED the calendar readings yet, sigh. He did quite well leading up to "Wise man, camel, the thing that he brought...another wise man, another camel, the thing that he brought." Hey, even many adults don't really know exactly what frankincense and myrrh are!)
So...life is about as normal as we can make it this year. Decorations are out of the basement and adorning shelves, mantles, and walls. The baking cupboard is bursting with supplies waiting to be mixed or melted and prepared for sharing and/or hoarding. While we've agreed as a family to drastically simplify our gift-giving this year, we still have special treats planned in the way of events and family activities, and the much-anticipated stockings will still hold treasures for eager hands (and mouths) to enjoy first thing Christmas morning.
In between trying to keep up with homeschool lessons and direct holiday activities, there are the not-so-normal bits...
* My OB appointment on Friday showed my belly measuring at the same point (23 cm) as at last month's appointment. (It should have been 28-29 with a baby growing at a standard rate.)
* I continue to monitor posts in the trisomy parents Facebook group. Wee ones have been stillborn or flown to the arms of Jesus in recent weeks. On the other hand, others are celebrating birthdays and milestones no one expected them to reach.
* Rhema weaned herself completely a couple of weeks ago. I'm thankful for a good nursing experience with her, one of our longest at 16 months (and definitely the longest I've nursed a baby while being pregnant!). But I couldn't help feeling a bit melancholy because of not knowing anything about what Verity's feeding needs will encompass.
* Any other year I'd be penciling in future events and looking forward with anticipation to things like traveling to our teens' speech/debate tournaments in the spring and my company convention in the summer. But now...my calendar remains blank with invisible question marks hovering over every possibility. Even local outings like concerts or plays are up in the air (for me at least, not necessarily the whole family). The only things I bother adding to my planner are ultrasound and OB appointments, knowing even those may change.
I'm in a kind of holding pattern, hovering closely enough to our final destination to feel the anticipation of finally landing and yet far enough away that I can't see the location with any clarity. I'm infinitely grateful that my Pilot's ways are higher than my ways, His thoughts higher than my thoughts (Isaiah 55:8-9). His perspective and purposes are eternal. He is perfect, and I can trust Him completely.
I have somewhat arrogantly assumed that our holiday season will be "normal," untouched by drama or trauma. Maybe it's wishful thinking; maybe it's an unspoken prayer that God will give us some sweet, precious memories together before Whatever Happens Next swoops in and takes over our lives. I desperately want to foster a festive and generous holiday spirit in our hearts and in our home, particularly for our younger children who don't have as many Christmas memories racked up as their older siblings. (I recently overheard my three-year-old son listing objects on our Advent calendar, having learned at least a few things even though we haven't actually STARTED the calendar readings yet, sigh. He did quite well leading up to "Wise man, camel, the thing that he brought...another wise man, another camel, the thing that he brought." Hey, even many adults don't really know exactly what frankincense and myrrh are!)
So...life is about as normal as we can make it this year. Decorations are out of the basement and adorning shelves, mantles, and walls. The baking cupboard is bursting with supplies waiting to be mixed or melted and prepared for sharing and/or hoarding. While we've agreed as a family to drastically simplify our gift-giving this year, we still have special treats planned in the way of events and family activities, and the much-anticipated stockings will still hold treasures for eager hands (and mouths) to enjoy first thing Christmas morning.
In between trying to keep up with homeschool lessons and direct holiday activities, there are the not-so-normal bits...
* My OB appointment on Friday showed my belly measuring at the same point (23 cm) as at last month's appointment. (It should have been 28-29 with a baby growing at a standard rate.)
* I continue to monitor posts in the trisomy parents Facebook group. Wee ones have been stillborn or flown to the arms of Jesus in recent weeks. On the other hand, others are celebrating birthdays and milestones no one expected them to reach.
 |
| https://www.facebook.com/groups/T18Mommies/ |
* Rhema weaned herself completely a couple of weeks ago. I'm thankful for a good nursing experience with her, one of our longest at 16 months (and definitely the longest I've nursed a baby while being pregnant!). But I couldn't help feeling a bit melancholy because of not knowing anything about what Verity's feeding needs will encompass.
* Any other year I'd be penciling in future events and looking forward with anticipation to things like traveling to our teens' speech/debate tournaments in the spring and my company convention in the summer. But now...my calendar remains blank with invisible question marks hovering over every possibility. Even local outings like concerts or plays are up in the air (for me at least, not necessarily the whole family). The only things I bother adding to my planner are ultrasound and OB appointments, knowing even those may change.
 |
| Image from www.sheknows.com/pregnancy-and-baby/day/53 |
I'm in a kind of holding pattern, hovering closely enough to our final destination to feel the anticipation of finally landing and yet far enough away that I can't see the location with any clarity. I'm infinitely grateful that my Pilot's ways are higher than my ways, His thoughts higher than my thoughts (Isaiah 55:8-9). His perspective and purposes are eternal. He is perfect, and I can trust Him completely.
Thursday, December 1, 2016
Farewell to Fall
It’s December, but I’m not quite ready to let go of November
yet. Perhaps the reason is a week-long trip our family took to San Antonio for
the National Bible Bee the week before Thanksgiving; we returned home Monday
the 21st and had to restock the fridge and pantry, do mountains of
laundry, and figure out what we were cooking for the Big Meal. We hosted my
parents, but honestly, it was a simple, quiet affair. I didn’t have time or
energy for the fun extras I usually enjoy doing. My birthday is November 22,
and I have always loved autumn. A favorite family tradition is adding to our “Blessing
Tree,” and I cherish the memories of little hands taping colorful paper leaves
to the branches and proclaiming gratefulness for everything from pizza and
stuffed animals to family and salvation in Jesus Christ.
 |
| One of the most normal shots of everyone; unfortunately, Rhema is not looking, but at least there are no bunny ears or crossed eyes...oh, wait. Tobin does have his eyes crossed. Sigh. |
This year we didn’t even set up the blessing tree. Our table was bare of adornment—we chose to do a buffet line. There was no need for place cards, so we didn’t bother. We used our special Blue Willow plates and went around the table several times saying what we were thankful for (no one was allowed to repeat anything already mentioned), but somehow it just seemed…incomplete. Somewhat disappointing, maybe even a bit hollow.
This isn’t fair to my amazing family. It was truly a joy to
spend a few days with my parents. The last time we had celebrated Thanksgiving
together was in 2009! And I had willing helpers in meal preparation (and more
or less willing helpers in clean-up, lol). The leftovers meant I didn’t have to
cook for a few days afterward, but a spell of possible salmonella put a huge
damper on the day after Thanksgiving as my poor hubby took to his bed with
stomach pains. (Thank the good Lord for Young Living’s DiGize essential oil
blend!)
 |
| We all thoroughly enjoyed the turkey, which we roasted in a paper bag, but: lesson learned, wash those ARMS, not just hands, after slathering butter and herbs all over the bird! |
Facebook now features a “See Your Memories” option, and I enjoy going back in time and seeing posts and photos from years past. There were several years when I joined with many others in posting something each day I felt thankful for. That fad seemed to be passé this year—maybe the political climate kept our attention elsewhere at the beginning of November? Or maybe folks in my Facebook feed, like me, simply decided not to do the daily posts. I certainly saw many beautiful sentiments of gratefulness: I enjoyed scrolling through photos of families gathered around tables, glimpses of culinary delights, and Bible verses proclaiming God’s goodness.
But—this year I have a new addition to my Facebook feed.
Posts to the trisomy parents support group show up randomly as I’m scrolling,
and I ended Thanksgiving evening in tears over a family who learned their baby
boy would be stillborn…doctors said they could have Thanksgiving with their
loved ones before going to the hospital for an induction. And this wasn’t the
only loss the trisomy community experienced during the holiday week.
So…with the turn of the calendar page to December, this
morning I am feeling reflective and somewhat melancholy. And yet—truly—my heart
overflows with Thanksgiving! This morning’s Bible reading for my husband and me
included a couple of chapters from Nehemiah, and I am reminded that in the
midst of mourning—indeed, in the midst of any circumstances—the JOY of the Lord
is our STRENGTH. And so, I write this as a final farewell to November 2016 and
the first Thanksgiving our family has experienced with a little person
named Verity in our lives.
Here is my list of 30 reasons I am thankful during this
unique time. In no particular order…I am thankful for:
- The fact that Verity is alive and kicking—this little girl is full of LIFE and certainly rivals her siblings in the gymnastics department!
- Advance notice of the Trisomy 18 diagnosis. Many families have no idea until after their little ones arrive. I am grateful God is allowing us this time of preparation.
- An incredibly supportive community of family and friends. I have never felt so loved and encouraged as I have over the past couple of months.
- A tenderhearted, like-minded husband. Truly, I could not be on this journey of life, love, and parenthood without my Ted, a man who not only holds me when I’m falling apart but is able and willing to cry along with me.
- Children who already treasure their unborn sister, speaking words of love and laughter to her through my expanding belly.
- The power and presence of God: there are days when I am amazed at what we are accomplishing in our homeschool routine, when I have joy and peace abounding for no other reason BUT GOD.
- The tender mercies of my Lord and Savior: there are days when I just “can’t even.” When I don’t shower and stay in my bathrobe and let the kids have whatever they find in the pantry to eat. When the best I can do is hang on for dear life until Ted gets home from work. And yet God’s power is made perfect as I wallow in weakness.
- The wonders of technology—ultrasounds that allow us to see Verity and keep tabs on her development.
- Verity’s wonderfully formed little body, knit together by a loving Creator.
- Coffee, made Italian-style by my husband every morning. It tastes delicious and never fails to make Verity dance.
- Medical professionals who embrace life no matter the diagnosis, and…
- Resources and encouragement beyond the medical professionals who don’t.
- New friends and connections I’ve made just in the last 2 months because of this journey we are on.
- Opportunities to speak life and truth to a hurting world.
- Opportunities to speak life and truth to our children, who are forming their own worldview.
- My new Instant Pot. (Now to find/make time to figure out how to use it so it can bless my family in the days to come…)
- A beautifully consistent heartbeat, heard on the monitor and seen on the ultrasound screen during each of Verity’s checkups so far.
- Verity’s beautiful little profile and healthy heart.
- Essential oils—not only are they keeping me and my family healthier than ever, but I also love purposefully praying and anointing my belly with oils like Frankincense and Lavender or blends such as Joy, Abundance, or Stress Away.
- The mental and emotional support I get each day from our oils…this is worth a separate mention, especially since a year ago I was struggling with some post-partum issues.
- The TRUTH of God’s Word, which reminds me that God’s thoughts and ways are higher than mine, and His purposes will prevail.
- The hope of eternity. Our struggles here are temporary and will fade away.
- My husband’s job that gives us health care coverage—knowing we do not have to make medical decisions based on whether or not we can afford them is a huge burden off our shoulders.
- A measure of normalcy in our lives—at least for now. Routine is good.
- A pretty “normal” pregnancy. Other than the T18 diagnosis, nothing about this pregnancy is really any different from my others, as far as my own physical health.
- Central air and heating. After living in Italy for 3 years and feeling hot in the summertime and freezing cold during the winter…well, I’m grateful.
- Our church. Everywhere we’ve been, God has put us in a community of believers who become our family. We know God placed us here “for such a time as this.”
- Peace. My heart is at peace, even though I yearn for insight into the future.
- Laughter. It really is “good like a medicine,” as Proverbs says. My husband and my kids make me laugh on a daily basis, and I am grateful!
- The truth of Hebrews 13:5 and 8, which reminds me that God will never leave or forsake us and that Jesus Christ is the same yesterday, today, and forever.
Subscribe to:
Posts (Atom)